Blastomycosis: A Fungal Infection with Hidden Dangers
Introduction:
Blastomycosis,(also known as Gilchrist’s disease) a fungal infection caused by the organism Blastomyces dermatitidis, is a relatively rare but potentially serious health concern. This infection primarily affects the lungs, but it can spread to other parts of the body, leading to a range of symptoms. In this article, we will explore the characteristics, causes, symptoms, diagnosis, and treatment of Gilchrist’s disease.
Understanding Blastomycosis:
Blastomycosis is caused by inhaling the spores of the fungus Blastomyces dermatitidis, which is commonly found in moist, wooded areas with rich organic matter. The spores become airborne when the soil is disturbed, such as during activities like excavation, construction, or outdoor recreational pursuits.
Symptoms of Blastomycosis:
- Respiratory Symptoms: The initial symptoms often resemble those of a respiratory infection, including cough, fever, and difficulty breathing. The infection primarily affects the lungs, leading to pneumonia-like symptoms.
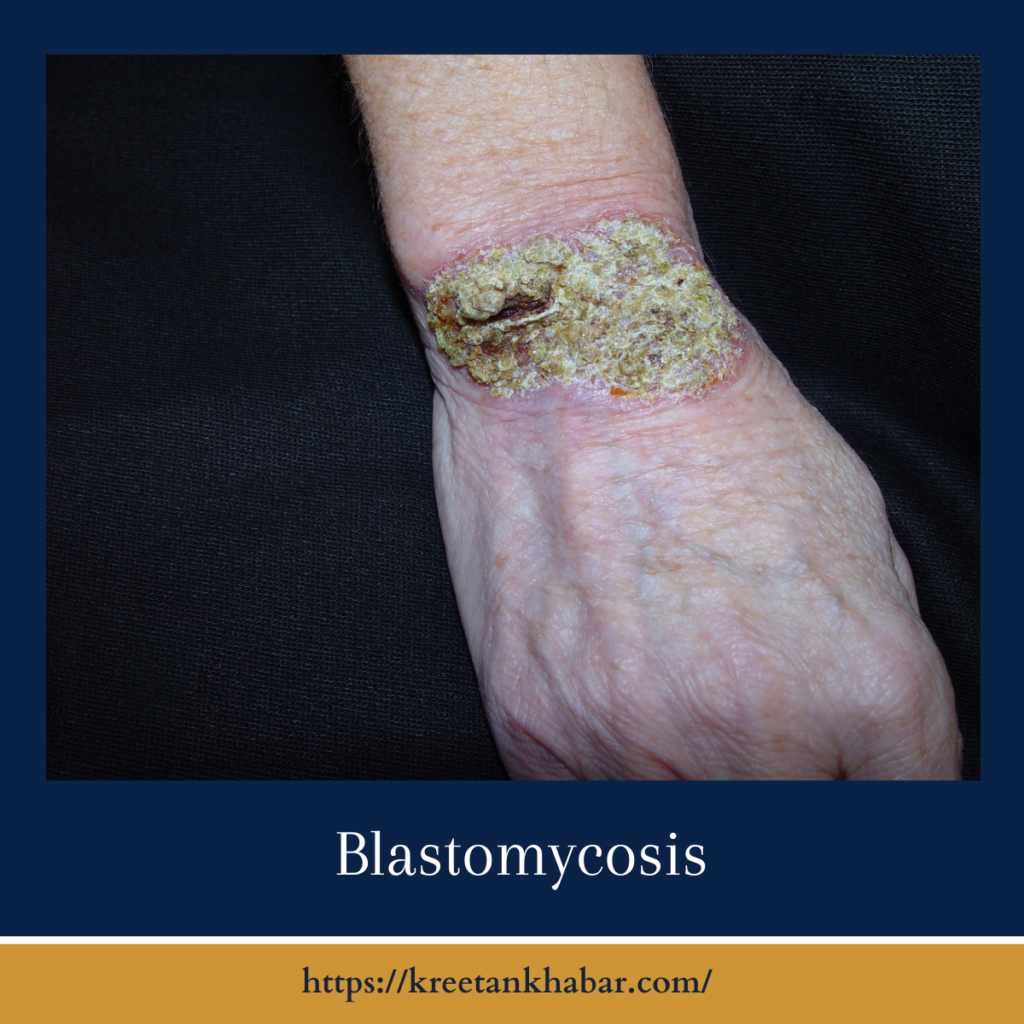
- Skin Lesions: In some cases, Gilchrist’s disease can spread beyond the lungs to other parts of the body, including the skin. Skin lesions, often resembling warts or ulcers, may develop. These skin manifestations can be one of the distinctive features of advanced Gilchrist’s disease.
- Fever and Chills: Systemic symptoms such as fever and chills are common, reflecting the body’s immune response to the fungal infection.
- Fatigue and Muscle Aches: Individuals with Gilchrist’s disease may experience fatigue and muscle aches, contributing to an overall sense of malaise.
- Joint Pain: Joint pain, swelling, and stiffness can occur, mimicking symptoms of arthritis. This is more likely in cases where the infection has disseminated to other parts of the body.
Diagnosis of Blastomycosis:
- Clinical Evaluation: A healthcare provider will conduct a thorough clinical evaluation, considering the patient’s symptoms, medical history, and potential exposure to environments where the fungus is prevalent.
- Chest X-ray: Imaging studies, such as chest X-rays, may reveal lung infiltrates and assist in the diagnosis of pulmonary Gilchrist’s disease.
- Cultures and Laboratory Tests: Cultures of respiratory secretions, skin lesions, or bodily fluids may be collected to identify the presence of Blastomyces dermatitidis. Laboratory tests, including fungal staining and microscopy, aid in confirming the diagnosis.
- Biopsy: In some cases, a biopsy of affected tissues may be necessary to confirm Gilchrist’s disease and rule out other potential causes of similar symptoms.
Treatment of Blastomycosis:
- Antifungal Medications: The primary treatment for Gilchrist’s disease involves antifungal medications, with itraconazole and voriconazole being commonly prescribed. Treatment duration may extend for several months, depending on the severity and extent of the infection.
- Amphotericin B: In severe cases or when the infection does not respond to initial antifungal therapy, healthcare providers may recommend intravenous administration of amphotericin B.
- Supportive Care: Supportive measures, such as pain management and addressing respiratory symptoms, may be employed to alleviate discomfort and improve the overall well-being of the patient.
The points about Treatment of Gilchrist’s disease:
Conclusion:
Blastomycosis, though uncommon, requires prompt recognition and treatment to prevent complications. Individuals living or spending time in regions where the fungus is endemic should be aware of the potential risks and seek medical attention if symptoms suggestive of blastomycosis arise. Early diagnosis and appropriate antifungal therapy significantly contribute to a positive prognosis for those affected by this fungal infection.
Read also : Exploring the Delightful Boost of the Green Tea Shot 2023