Thrombocytopenia: A Closer Look at Low Platelet Counts
Introduction:
Thrombocytopenia, a term that might sound unfamiliar to many, is a medical condition characterized by a lower than normal platelet count in the blood. Platelets are tiny, disc-shaped blood cells that play a crucial role in clotting and preventing excessive bleeding. When the platelet count drops below the normal range (typically less than 150,000 platelets per microliter of blood), it can give rise to various complications.
Understanding Platelets:
Before delving into the intricacies of thrombocytopenia, let’s appreciate the role of platelets in the human body. Platelets are produced in the bone marrow and are essential for blood clotting. In response to injury, platelets rush to the site, adhere to the damaged blood vessel walls, and initiate the clotting process. This prevents excessive bleeding and promotes wound healing.
Causes of Thrombocytopenia:
The causes of thrombocytopenia are as diverse as the conditions that shape our health landscape. A complex interplay of factors can disrupt the delicate balance of platelet production and function. Bone marrow disorders, such as leukemia and aplastic anemia, can throw a wrench in the intricate machinery responsible for creating these tiny blood cells. On another front, the immune system may occasionally go rogue, mistakenly attacking and destroying platelets, giving rise to immune thrombocytopenic purpura (ITP).
Viral invaders, including HIV and hepatitis C, can also influence platelet production or incite immune responses that contribute to thrombocytopenia. Medications, often intended to heal, may paradoxically lead to a drop in platelet counts as a side effect. Additionally, rare genetic disorders add another layer of complexity to this intricate puzzle. Unraveling the web of causes behind thrombocytopenia requires a keen investigative spirit in the realm of medicine, where understanding the nuances of each case becomes paramount for effective diagnosis and tailored treatment.
Thrombocytopenia can be caused by a multitude of factors, ranging from underlying medical conditions to medications and lifestyle choices. Here are some common causes:
- Bone Marrow Disorders: Conditions such as leukemia, myelodysplastic syndromes, and aplastic anemia can affect the bone marrow’s ability to produce an adequate number of platelets.
- Immune System Disorders: In some cases, the immune system may mistakenly attack and destroy platelets, leading to thrombocytopenia. This condition is known as immune thrombocytopenic purpura (ITP).
- Viral Infections: Certain viral infections, such as HIV, hepatitis C, and Epstein-Barr virus, can impact platelet production or trigger immune responses that result in thrombocytopenia.
- Medications: Some medications, including certain antibiotics, anticonvulsants, and diuretics, can cause a decrease in platelet counts as a side effect.
- Genetic Factors: Rare genetic disorders, like Wiskott-Aldrich syndrome and May-Hegglin anomaly, can contribute to thrombocytopenia.
Symptoms and Complications:
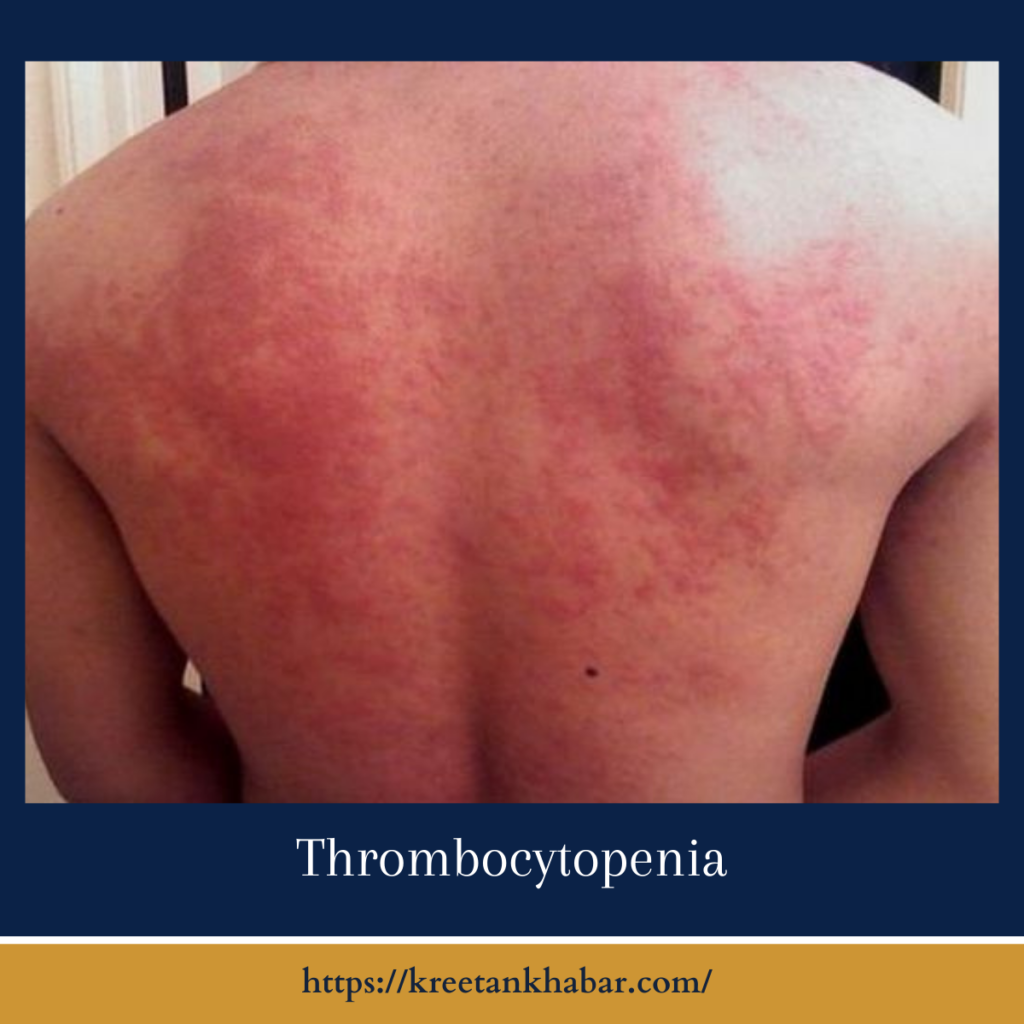
Thrombocytopenia manifests in a spectrum of symptoms that can range from subtle to potentially life-threatening. One of the early signs is easy bruising, where even minor bumps result in noticeable discoloration. Petechiae, those small, red or purple spots on the skin, become apparent due to tiny blood vessel bleeding. Individuals may also experience prolonged bleeding from minor cuts or mucous membranes. These symptoms underscore the challenges of compromised platelet function.
In severe cases, thrombocytopenia can lead to more ominous complications, including internal bleeding and hemorrhage. It’s a delicate balance, as the symptoms serve as red flags, urging timely medical attention to prevent the progression of complications. Understanding these warning signs is paramount in navigating the complexities of thrombocytopenia and seeking appropriate care to safeguard against its potentially serious consequences.
Thrombocytopenia may go unnoticed initially, as mild cases often exhibit no symptoms. However, as the condition progresses, individuals may experience:
- Easy bruising: Due to a lack of platelets, even minor bumps or injuries can lead to bruising.
- Petechiae: Small, red or purple spots on the skin, resulting from tiny blood vessel bleeds.
- Excessive bleeding: Prolonged bleeding from minor cuts or mucous membranes.
Severe cases of thrombocytopenia can lead to life-threatening complications, including internal bleeding and hemorrhage.
Diagnosis and Treatment:
Diagnosing and treating thrombocytopenia is a multifaceted process that requires a careful examination of the underlying factors contributing to low platelet counts. The initial step involves a comprehensive assessment, including a detailed medical history and physical examination. Blood tests play a pivotal role in quantifying platelet levels and identifying potential causes, whether they stem from bone marrow disorders, immune system malfunctions, viral infections, or medication side effects. Once diagnosed, the treatment approach varies depending on the severity and root cause of thrombocytopenia.
Addressing the underlying conditions, such as managing infections or correcting bone marrow abnormalities, is often a primary focus. In cases where immune-related thrombocytopenia is a concern, medications like corticosteroids may be prescribed to modulate immune responses. For severe instances where there’s a heightened risk of bleeding, platelet transfusions can be administered. Striking a balance between addressing the immediate symptoms and targeting the root cause is crucial in formulating an effective treatment plan for individuals grappling with thrombocytopenia.
Diagnosing thrombocytopenia involves a thorough medical history, physical examination, and blood tests to measure platelet counts. Treatment depends on the underlying cause and the severity of the condition:
- Addressing Underlying Conditions: Treating the root cause, such as managing infections or correcting bone marrow disorders, is essential.
- Medications: In some cases, corticosteroids or other immune-modulating drugs may be prescribed to manage immune-related thrombocytopenia.
- Platelet Transfusions: In severe cases, especially when there is a risk of significant bleeding, platelet transfusions may be necessary to raise platelet counts.
- Lifestyle Modifications: Avoiding medications that contribute to thrombocytopenia and making certain lifestyle changes, such as avoiding alcohol and adopting a balanced diet, may also be recommended.
More points of diagnosis and treatment:
- Comprehensive Evaluation: Diagnosing thrombocytopenia kicks off with a thorough assessment, including a detailed medical history and physical examination. Understanding the patient’s health journey becomes crucial in identifying potential triggers for low platelet counts.
- Blood Tests for Precision: Blood tests play a pivotal role in quantifying platelet levels and uncovering the specific factors contributing to thrombocytopenia. This precision allows healthcare professionals to tailor treatment plans based on the root cause.
- Targeting Underlying Causes: Treatment strategies hinge on addressing the underlying conditions. Whether it’s managing infections, correcting bone marrow disorders, or mitigating the impact of immune system malfunctions, a targeted approach aims to restore the delicate balance of platelet production.
- Immunomodulation: In cases where the immune system is the culprit, medications like corticosteroids may be prescribed to modulate immune responses. This approach seeks to alleviate the immune-related factors contributing to thrombocytopenia.
- Platelet Transfusions: In situations where there’s an immediate risk of severe bleeding, platelet transfusions become a crucial intervention. This involves infusing donated platelets into the patient’s bloodstream to elevate platelet counts rapidly.
- Lifestyle Considerations: Beyond medical interventions, lifestyle modifications play a role. Avoiding medications that exacerbate thrombocytopenia and adopting a balanced diet contribute to a holistic approach in managing the condition.
- Monitoring and Adjusting: Given the nuanced nature of thrombocytopenia, continuous monitoring is essential. Treatment plans may need adjustment based on the patient’s response and the evolving dynamics of their health.
- Patient Education: Empowering individuals with thrombocytopenia with knowledge about their condition, its triggers, and the importance of adherence to treatment plans is a cornerstone in managing this complex hematologic disorder.
- Collaborative Care: The diagnosis and treatment of thrombocytopenia often require a multidisciplinary approach, involving hematologists, immunologists, and other specialists. Collaborative care ensures a comprehensive and well-coordinated strategy for optimal patient outcomes.
Conclusion:
Thrombocytopenia, though often unfamiliar to the general public, is a condition that warrants attention and understanding. Awareness of the causes, symptoms, and available treatments is crucial for both individuals affected by thrombocytopenia and the healthcare professionals managing their care. Through continued research and education, we can strive to demystify this condition and pave the way for improved diagnosis and treatment strategies.
Read also : Exploring the Delightful Boost of the Green Tea Shot 2023